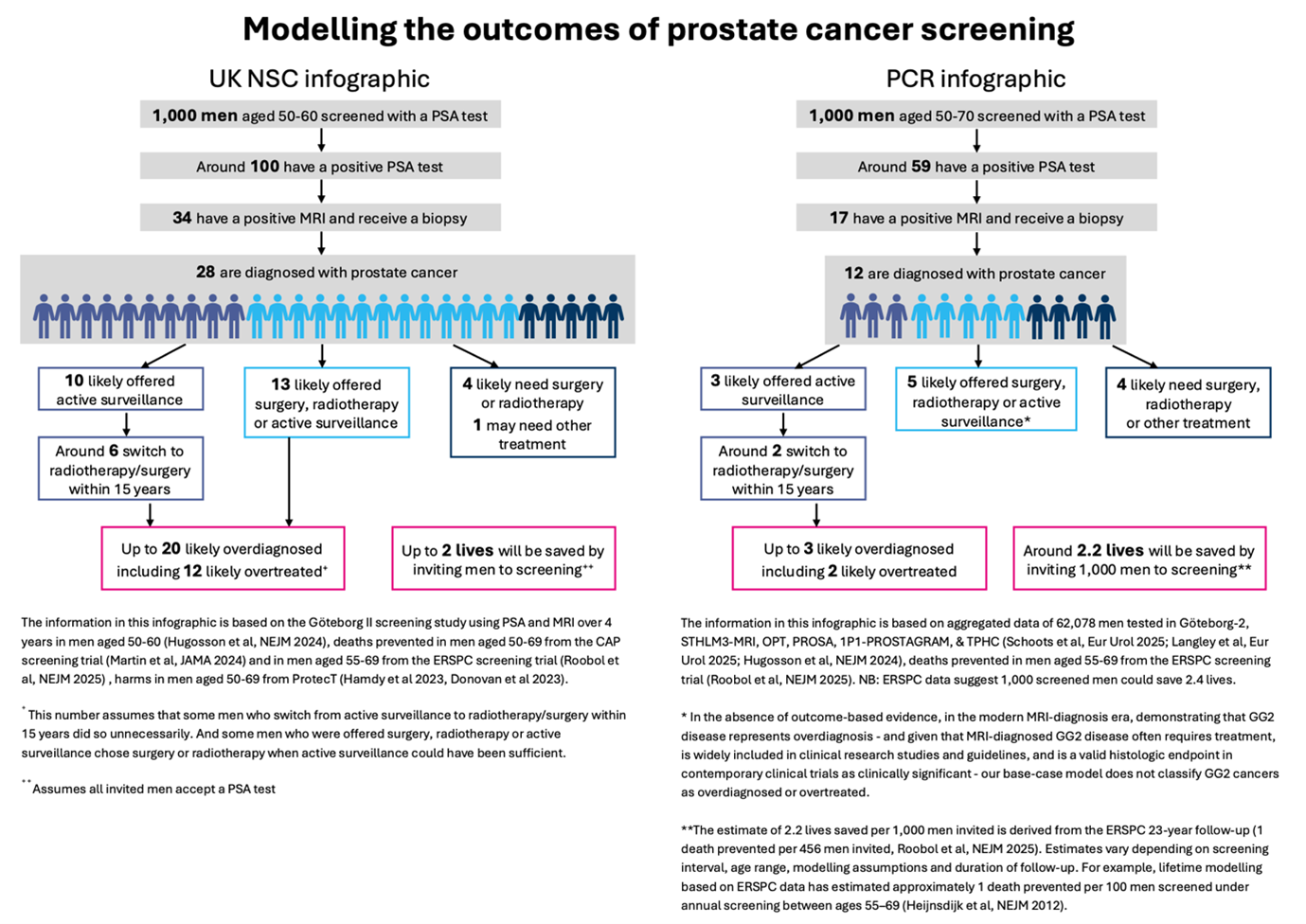
A copy of PCR’s infographic comparison can be downloaded here: https://www.prostate-cancer-research.org.uk/wp-content/uploads/2026/02/Prostate-cancer-screening-infographic-PCR-alternative-Feb-2026.pdf
Decision to deny prostate cancer screening based on flawed economic model, independent review finds
- An independent review has identified structural flaws in the economic model used to justify blocking the introduction of a national prostate cancer screening programme.
- The model relies on outdated data, fails to account for the impact of a coordinated screening programme on the UK’s existing testing landscape, and does not address serious population health inequalities.
- Analysis of contemporary MRI-led screening studies suggests that the harms cited by the UK National Screening Committee (UK NSC) may be substantially overstated.
- Charities and experts are calling for the model to be rebuilt to enable a fair assessment of screening before any final recommendation by the UK NSC.
[London, UK] A new independent review by the York Health Economics Consortium (YHEC), commissioned by Prostate Cancer Research (PCR), has uncovered significant structural failings in the model used by the UK National Screening Committee (UK NSC) to justify its recent draft recommendation against the introduction of a national prostate cancer screening programme.
PCR is calling for an extension to the UK NSC’s review process to allow the model to be structurally rebuilt, with greater use of contemporary NHS data and modern diagnostic pathways, before a final decision is reached.
New analysis suggests markedly lower overdiagnosis under modern pathways
An infographic published by the UK NSC states that for every life saved by a screening programme, 10 men would be overdiagnosed and 6 would be overtreated.
However, PCR’s analysis of six contemporary studies encompassing over 62,000 men and reflecting modern MRI-led pathways, which more accurately reflect real-world UK practice, suggests substantially lower harms. Across these studies, approximately 1.5 men were overdiagnosed and around 1 overtreated for every life saved – a reduction of up to seven-fold compared with the figures cited by the UK NSC.
These findings suggest that harms associated with screening in the current NHS context may be significantly lower than those projected in the UK NSC model, which draws heavily on decades-old trial data representing historic screening pathways.
UK NSC model treats screening as “additional” cost rather than reform of existing testing
The economic model – produced by the Sheffield Centre for Health and Related Research (SCHARR) – assumes that a screening programme would operate in addition to the UK’s current opportunistic PSA testing landscape, thereby adding new costs and harms rather than as a partial or full replacement of the existing activity.
Currently, hundreds of thousands of PSA tests are performed annually in asymptomatic men through ad-hoc, patient-initiated testing.[1],[2] Experts describe this approach as inconsistent and poorly targeted, with more men in their 80s being tested than those in their 50s – the group most likely to benefit from early detection.
In countries such as Lithuania, the introduction of an organised screening programme reduced unnecessary testing in older men by approximately 80%. However, the SCHARR model assumes no reduction in opportunistic testing following the implementation of organised screening.
By modelling screening as an entirely new cost layered on top of existing activity – rather than as a reform of current practice – the model inflates projected costs and harms.
Furthermore, the model assumes only 36% of men would attend screening. In contrast, a recent nationally representative Healthwatch England poll found that 79% of men (and 81% of Black men) would likely attend if invited.[3] Higher participation would materially affect both projected benefits and cost-effectiveness estimates.
Outdated data used and health inequalities ignored
The YHEC review highlights that the model relies heavily on outdated diagnostic and treatment assumptions derived from trials conducted before the routine use of modern MRIs and active surveillance.
It also fails to account for:
- The shift from more expensive MRI scans to cheaper, faster MRI now in practice across the NHS,[4] and
- The long-term costs of treating advanced, metastatic cancer, particularly as modern drugs now extend survival.
PCR shared independent modelling conducted by Deloitte indicating that the lifetime treatment costs for a man diagnosed with stage 4 prostate cancer may be in the region of £127,000 – higher than the assumptions used in the UK NSC’s model.[5]
Furthermore, while Black men face approximately double the lifetime risk of prostate cancer, the model does not meaningfully assess how an organised programme could reduce inequalities embedded within the current system. Cost-effectiveness estimates for Black men are already close to the accepted threshold in the model, meaning even modest adjustments to reflect modern practice could tip the scales in favour of screening this group.
As part of its independent review, YHEC requested that additional scenarios be tested within the existing model. When applied, several screening strategies – particularly for Black men and men with a family history – fell below the threshold used by the UK NSC to determine cost-effectiveness.
This demonstrates that when contemporary and clinically plausible assumptions are applied to the model, the conclusions change materially. Where reasonable experts disagree, and where alternative assumptions change the results, the current conclusion cannot be considered definitive. The model must therefore be fundamentally revised and strengthened before any final recommendation is made.
Oliver Kemp MBE, CEO at Prostate Cancer Research, said:
“Prostate Cancer Research is deeply concerned by the narrowness of the draft recommendations, which fail to tackle the harms inherent in the current system and leave men of Black ethnicity and those with relevant family history continuing to rely on current routes for testing.
“We are not arguing that screening is without risk, nor do we dispute the findings of historic trials that evaluated earlier forms of screening. Our concern is that the current model overly relies on this historic data and in doing so does not sufficiently reflect how prostate cancer is diagnosed, managed, and treated in the NHS today.
“When contemporary MRI-led pathways and real-world NHS data are considered, projected harms appear substantially lower.
“Given that this decision will shape prostate cancer early detection policy across the four UK nations for years to come, it is essential that the modelling framework reflects modern clinical practice and current health inequalities before any final recommendation is made.
“We strongly believe the review on this critical issue should be extended to allow time for amendments to the economic model to be made and fully tested. This crucial decision should not be based on a version of screening from decades ago.”
PCR is urging the UK NSC to rebuild the model to ensure that its final decision is based on a fair and contemporary assessment of risks, costs and benefits.
To ensure this issue remains at the top of the government’s agenda, PCR is calling on members of the public to sign its Parliamentary e-petition to trigger a formal debate in Parliament.
Sign the petition here: https://petition.parliament.uk/petitions/751472
ENDS
[1] Prostate Cancer Research. Prostate Cancer Screening: Impact on the NHS; 2025
[2] Collins KK, Oke JL, Virdee PS et al. Prostate specific antigen retesting intervals and trends in England: population based cohort study. BMJ. 2025 Oct 8;391:e083800. doi: 10.1136/bmj-2024-083800.
[3] https://www.healthwatch.co.uk/blog/2025-10-08/men-would-come-forward-prostate-cancer-screening
[4] Strieder de Oliveira G, Altmayer S, Torri GB et al. Diagnostic Performance of Biparametric versus Multiparametric Magnetic Resonance Imaging for Prostate Cancer Diagnosis: An Updated Systematic Review and Meta-analysis, Eur Urol (2026) doi: 10.1016/j.eururo.2026.01.030
[5] Prostate Cancer Research. Socio-economic Impact of Prostate Cancer Screening; 2024
Notes to editors:
- Media contact: Jess Farmery [email protected]
- Prostate Cancer Research contact: David James [email protected]
- Sign Prostate Cancer Research’s e-petition to help secure a Parliamentary debate on screening: https://petition.parliament.uk/petitions/751472
- Patient case studies and expert spokespeople available on request
- Key statistics:
- Prostate cancer is the most common cancer in UK men (63,000+ diagnoses/year) and is the cause of 12,000 deaths annually (i).
- Targeted screening would cost approx. £25m/year (0.01% of NHS budget) (ii).
- Late-stage treatment costs 10x more than early-stage treatment (£127k vs £13k) (iii).
- A Healthwatch England poll found that 79% of men would attend screening if invited (iv).
- A copy of YHEC’s independent report can be downloaded here: https://www.prostate-cancer-research.org.uk/wp-content/uploads/2026/02/PCR-Prostate-Cancer-Model-Critique-19.02.26.docx
A copy of Prostate Cancer Research’s full submission can be downloaded here: https://www.prostate-cancer-research.org.uk/wp-content/uploads/2026/02/UKNSC-review-on-prostate-cancer-screening-PCR-response-20022026.pdf
Confirmed Co-signatories
- Black Equity Organisation
- Black Prostate Cancer Network
- British Association of Urological Nurses
- Cancer Black Care
- Cancer Don’t Let It Win CIC
- Can-Survive UK
- Caribbean & African Health Network
- CHAPS
- From Me To You: The Art of Survival CIO
- Help Educate and Raise Awareness Around Cancer CIC
- Orchid
- Prost8 UK
- Prostate Cymru
- Tackle Prostate Cancer
- The Bob Willis Fund
- The Graham Fulford Charitable Trust
- The Prostate Project
- The Rose Thompson Foundation